Study led by Pr Sébastien Froelich, neurosurgeon at Lariboisière hospital, Paris.
It is recalled that ACP = Cyproterone acetate = Androcur
Context: the behavior of meningiomas under the influence of progestin treatment is still unclear.
Objective: to study the relationship between the kinetics of growth of intracranial meningiomas and the use of cyproterone acetate progestogen (ACP)- Androcur
Methods : This study prospectively followed 108 women with 262 intracranial meningiomas and documented use of ACP. An analysis by meningioma was carried out. The volume changes of meningiomas over time and the growth speeds of meningiomas have been measured by magnetic resonance imaging (MRI) after stopping the ACP.
Results : the average duration of follow-up was 30 (standard deviation [and] 29) months. Ten (4%) meningiomas were treated surgically to the presentation. The other 252 Méningiomes were followed after stopping treatment with ACP. Overall, the followed meningiomas have decreased their volume by 33 % on average (standard deviation 28 %). In total, 188 (72 %) meningiomas decreased, 51 (19 %) meningiomas remained stable, and 13 (5 %) increased in volume, 3 (1 %) of which were treated surgically due to radiological increase during the follow -up after the withdrawal of the ACP. A total of 239 meningiomas out of 262 (91 %) regressed or stabilized during follow -up. Analysis in subgroups in 7 women with 19 meningiomas with a follow-up before and after the withdrawal of the ACP demonstrated that the speed of growth of the meningiomas has changed in a statistically significant way (p = 0.02). The meningiomas increased (average speed of 0.25 mm3/day) while the patients used the ACP and decreased (average speed of -0.54 mm3/day) after stopping the ACP.
Conclusion : 91 % of intracranial meningiomas in patients who used cyproterone acetate for a long time decrease or stabilize to MRI after stopping ACP treatment. Meningioma growth kinetics changes significantly, going from growth during the use of ACP to narrowing after the withdrawal of the ACP.
Keywords: meningioma, progesterone, volumetric MRI
The biological relationship between the growth of meningiomas and sex hormones is the subject of a debate. A relationship between progesterone and the growth of meningiomas seems likely in view of the following results. The meningiomas have a female predominance, as shown in the women-men's report of 2: 1. The meningiomas have an acceleration of tumor growth during pregnancy and a narrowing after childbirth. Eighty percent of meningiomas express progesterone receptors. These receptors are overexpimized in meningiomas compared to the normal meningeal fabric, and the expression of progesterone receptors in meningiomas is higher in women. A relationship between the growth of meningiomas and exogenous progestins also seems likely. Recently, a national cohort study in France has shown that women treated with the progestogen Acetate of Cyproterone (ACP) or Androcur® (Bayer Pharmaceuticals, Leverkusen, Germany) presented a risk of 7 to 20 times higher to develop a meningioma. The PCA is prescribed for hyperandrogenism, contraception, ovarian dysfunction, and several other indications in European countries, including France and the United Kingdom. In addition, several cases have shown regression of meningiomas after stopping the ACP. This study examines the kinetics of the growth of meningiomas in relation to the use of ACP in a series of cases of adult women who used ACP for various indications, but mainly for hyperandrogenism. The objective is to consolidate the hypothesis that meningiomas develop during the use of progestins and stabilize, or even decrease in size, once the progestins are stopped.
METHOD
Ethical approval
This study was approved by the local ethics committee of the neuroscience pole of the Lariboisière hospital, Paris, France. The written consent of patients for inclusion in this study has been obtained and recorded.
Inclusion and exclusion criteria
from a database prohibited prospectively with patients referred to external consultation due to intracranial meningiomas and the use of ACP, we have retrospectively a population of patients suitable for analysis in this study.
The following inclusion criteria were made. Patients had to present the following elements:
- Presence of at least 1 intracranial meningioma,
- Documented use of ACP,
- Presence of at least 2 sequential examinations of magnetic resonance imaging (MRI) of the brain with 3D T1 sequences reinforced by gadolinium, (MRI) sequential cerebral with 3D T1 sequences reinforced by gadolinium,
- Presence of at least one brain MRI carried out after stopping the use of ACP.
The exclusion criterion was a history of co-statement of nomegestrol
nomegestrol nomegestrol.
Characteristic of meningiomas
An analysis by meningioma has been carried out. For each meningioma, the following characteristics have been collected: laterality, general location, precise location, MRI dates, and MRI volumes. In addition, any occurrence of radiotherapy/radiochuruse has also been noted.
Surgery and radiotherapy
Surgery, indication of surgery, the grade of the tumor, hormonal receptors and radiotherapy/radiosurgery have been noted.
Definitions of the location of meningiomas
The location of meningiomas was divided into 5 categories: anterior, medium and posterior cranial pit, convexity and midline.
These 5 general locations were subdivided into several specific locations. The anterior cranial pit included the meningiomas of the orbital roof, the sheath of the optic nerve, the olfactory groove, the anterior clinoid, the plann and the Sellae tuberculum. The average cranial pit included the cavernous sinus, the sphenoid wing, the spheno-orbital and the authentic meningiomas of the average pit. The posterior cranial pit included the ponto-cerebellar angle and the tentoral meningiomes.
The convexity category included meningiomas of front, parietal and temporal convexity. The midline category included parasagittal and falx meningiomas.
Volume of meningiomas
for each meningioma, we calculated the volumetric differences between different points over time during follow -up. The “percentage of volumetric difference after withdrawal of the ACP”, or DPPOST ACP, is defined in Formula 1:
DPPOST PCA = DVPost PCA ÷ VDATE D'Or stop × 100%, (1)
Where vstop Date is the volume of meningioma on the MRI performed closest in time of the date of withdrawal of ACP, while DVPOST ACP is the "post -volumetric difference post withdrawal" defined by the following formula volumetric difference after the withdrawal of the ACP "defined in Formula 2:
DVPost PCA = Vstop Date -VOFINAL Date, (2).
Where Vfinal Date is the volume of meningioma on the MRI made during the last follow -up. In addition, the "percentage of volumetric difference after the withdrawal of the ACP withdrawal from the ACP" was used to define a categorical variable in order to translate in a more intuitive way the way in which a meningioma responded volumetrically to the stop of the ACP. This variable is called "volumetric response".
The volumetric response has 3 possible values, namely "decrease", "stable" or "increase".
or "increase", which are defined below.
Volumetric response:
- Decrease: DPPOST ACP <(-Einterrate),
- Stable: (Einterrate)> Dppost ACP <(-einterrate),
- Increase: DPPOST ACP> (Einterrate), where it is the average percentage of inter-jugs more 2 standard deviations (and). Standard (SDS). Each meningioma has been categorized accordingly.
Méningiomes velocity
in addition, the speeds of meningiomas have been calculated. The "speed of meningioma after withdrawal of the ACP", or MVPOST ACP, was calculated according to Formula 3:
MVpost ACP = DVPOST ACP ÷ DTPOST ACP, (3)
where DTPOST ACP is defined as the time difference (in days) between the date of the MRI performed closest to the date of withdrawal of the ACP, and the date of MRI.
Volume measures
The volumetric measures were carried out with the PACS Viewer software (Carestream version 12.1.6.0116; Carestream Health Inc, Rochester, New York). The outline was manually produced, slice per slice, by 2 neurosurgeon certified on the basis of the image of the hospital. by 2 neurosurgeons certified on the 3D T1 axial MRI sequences reinforced in Gadolinium. 3D axials improved by gadolinium. The volume of meningioma used in all analyzes was the average of the volumes of the two assessors. Average of the volumes of the two assessors.
Selection of subgroups
A specific subgroup has been selected to answer the question of whether there is a difference in the growth speed during use and after removing ACP in the same patients. The additional criteria for selecting the subgroup were as follows
- Presence of at least 2 brain MRI acquired during the use of ACP,
- Presence of at least 1 brain MRI after stopping the ACP.
See table in the study link page 3
Statistical analysis
Linear regression analyzes were carried out with IBM SPSS Statistics (version 25; Armonk, New York). The non -adjusted R2 and R2 values are indicated. For the analysis of subgroup, a paired bilateral T test was carried out to compare the "speed of meningioma during ACP treatment" with the "speed of meningioma after the withdrawal of the ACP". A value p <0.05 was considered to indicate a significant difference.
Participating
results Our database contained 132 patients. In this 112 patient database met the inclusion criteria. 20 patients were not included because they did not have 2 sequential sequential MRIs with sequences reinforced by the T1 weighting gadolinium at the time of the analysis. Four patients were excluded due to the co-use of nomestrol acetate. Finally, the data of 108 women with a total of 262 meningiomas were analyzed . The average monitoring period was 30 ± 29 months (median: 18 months).
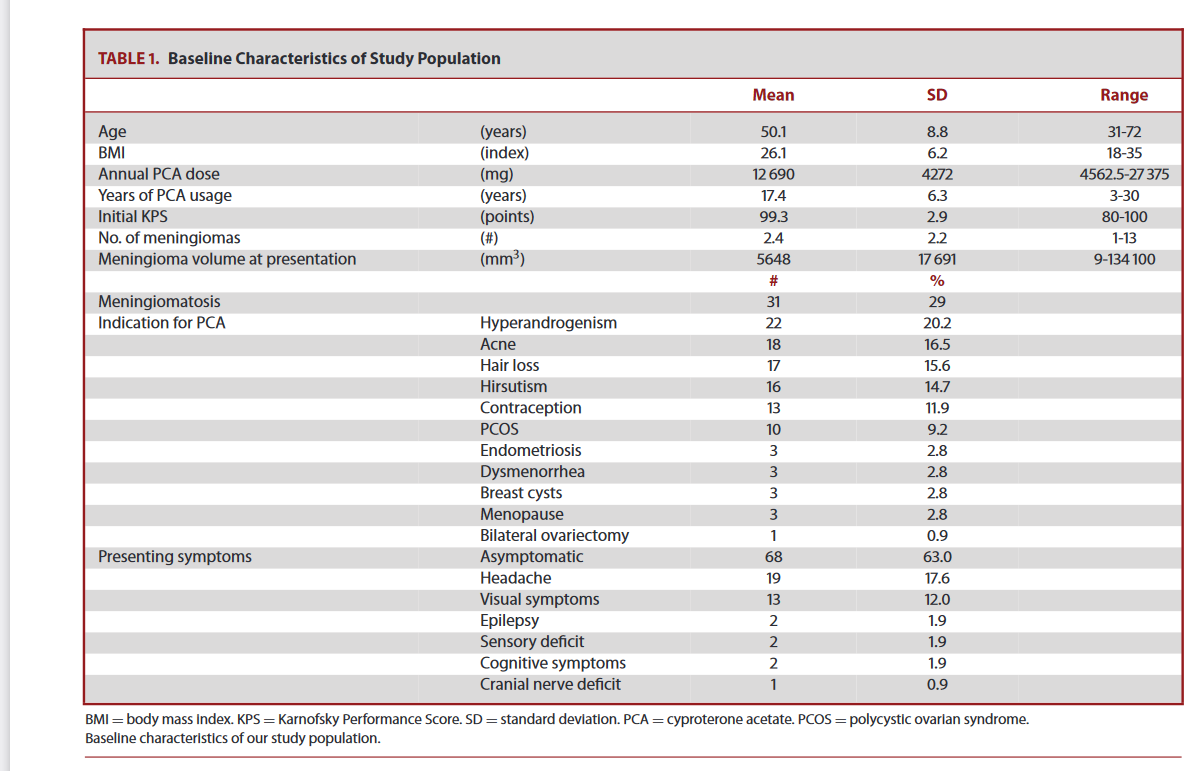
Basic characteristics
The results of the basic measurements are presented in Table 1. All patients were women. The average age of the participants was 50 (SD 9) years, and their average body mass index (BMI) was 26 (standard deviation 6). The women's site were processed with a daily dose of ACP between 25 and 75 mg, corresponding to a 25 and 75 mg, which corresponded to an average annual ACP dose of 12,690 (and 4272) MG, with an average duration of use of 18 (and 6.4) years. The most frequent indications for the prescription of ACP were hyperandrogenis (20.2 %) and the symptoms associated with it, such as acne (16.5 %) or hair loss (15.6 %). About 11.9 % of women used ACP for contraception. However, the choice of ACP was also partly based on additional signs of hyperandrogenism in this category of patients. category of patients. The patients had an average of 2.4 (standard deviation 2.2) meningiomas, and 29 % met the criteria of meningimatosis (defined by the presence of 3 or more meningiomas). Most patients were asymptomatic (63%) or had headache (18%) as initial symptoms.
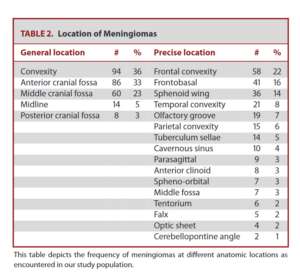
The ochalization of meningiomas
The results for the locations of meningiomas are given in Table 2.. The most common location of meningiomas was convexity (36 %) and the previous cranial pit (33 %), and the most common specific location was frontal convexity (22 %).
See table in the study link page 4
Surgery and radiotherapy
ten (3.81 %) meningiomas in 9 patients were operated within 3 months of the presentation and within 3 months of stopping the ACP due to progressive symptoms. Three (1.2 %) meningiomas were operated due to radiological increase despite stopping the ACP. Twelve were meningothelial meningiomes of Grade I of the WHO, and 1 was a transitional Mes I. Mesningioma. All had an expression of the progesterone receptors. The Ki-67 marking index was between 1% and 4%. Three meningiomas (1.15 %) were irradiated in 2 patients. The first patient had a meningioma of the cavernous sinus, initially irradiated irradiated with photons during the ACP treatment, then operated shortly after the presentation. The other patient had 2 meningiomas (optical sheath and temporal convexity). Optical sheath and temporal convexity) which received an irradiation to protons 5 years after the withdrawal of the ACP due to a progressive visual loss.
Inter Correspondence Judged
the 2 evaluators had an average relative difference between the volume measures of 2.1% (SD 3.4). Consequently, the value of the interesting (see the methods section) to determine the volumetric response has been calculated at 9 %.
Volumes and speed of meningiomas
An analysis of the volumes was carried out for 252 meningiomas. Ten meningiomas (3.8 %), operated during the presentation, were excluded. There has been an overall decrease in the volume of -1628 (SD 6924) MM3, or -33.2 (SD 34.4)%, and a "narrowing" or a negative growth speed of -5.8 (SD 28.3) mm3/day, or -2.1 cm3/year, after stopping ACP treatment. The figure shows the results of volumetric analysis. In terms of volumetric response (see the Methods for Definition), 188 (71.76 %) Méningiomes decreased, 51 (19.46 %) Méningiomes remained stable and 13 (4.96 %) increased after stopping ACP treatment. A linear regression modeling (Table 3) was carried out to predict the speed of growth of meningiomas after stopping treatment with ACP from the following parameters: meningimatosis, quantity of meningiomas, years of use, cumulative dose, BMI, age, general location, precise location and meningiomal departure volume. Univariate modeling has been used to select the variables for a multiviated model. The following variables have proven to be added significantly (p <0.05) to the prediction of the growth speed of meningomes during univariate modeling: number of meningiomas (R2 = 0.17, p = 0.04), presence of meningimatosis (R2 = 0.03, p = 0.01), precise location (R2 = 0.02, p = 0.02) and starting volume of meningiomas (R2 = 0.2, p = 0.00). During multivariate modeling, a significant regression equation was found F (4, 254) = 17.65, p = .000, with an R2 of 0.22. Only the starting volume of meningioma (t = -7.39, p = .00) has remained a statistically significant predictor (p <0.05). See Table 3 for more details on regression models.
Results of the sub-groups
in addition, 7 patients with a total of 19 meningiomas were included in the analysis of subgroup to answer the question of whether there is a difference in the growth speed during use and after stopping the ACP. The average age of the subgroup was 49 (SD 7) years. The average BMI was 26 (standard deviation 6). The sub-group was treated with a daily dose of PCA of 25 or 50 mg, corresponding to an average annual dose of ACP of 9033 (SD 248) MG, with an average use period of 18 (SD 4) years. Patients had an average of 2.7 (SD 2.0) meningiomas, and 38% had meningimatosis. About 83 % were asymptomatic or had headache (17 %) as symptoms. During the use of ACP, the overall growth of meningiomas was 0.25 (SD 0.45) mm3/day, while after stopping treatment, a global narrowing of meningiomas of -0.54 (SD 1.26) mm3/day was observed. This growth speed change was statistically significant (p = 0.02 in a bilateral t test of paired samples).
Discussion
The results presented suggest that the use of exogenous progestogen influences the kinetics of growth of intracranial meningiomas in adult women . The modeling of regression has shown that the initial volume of meningioma significantly predicts the speed of growth of meningioma after stopping the ACP . This seems logical because a greater volume of meningioma leads to a relatively greater growth or narrowing. During multivariate analysis, this effect surpassed the effect of the quantity of meningiomas, the presence of meningiomatosis and the precise location of meningiomas, which were significant in univariate modeling.
See table in the study link page 5

Comparison with previous studies
The natural history of "accidental" meningiomas without documented exhibition to progestins has been the subject of numerous studies. About 70 to 75 % of these meningiomas have growth over time and 25 to 30 % do not develop significantly.
Different growth models (for example, linear, exponential, linear, exponential or sigmoid) have been identified. The narrowing of meningiomas has been described but is a rare phenomenon. In comparison, the results presented in this series of meningiomas associated with the APC are surprisingly different from previous reports on "accidental" meningiomas. For example, Oya et al reported that in a study of 244 patients with 277 meningiomas, 44% of meningiomas increased during monitoring from 3 to 4 years. From 3 to 4 years old, and no regression of meningiomas was observed.
Conversely, after stopping treatment with ACP, the meningiomas of this series increased in 5 % of cases and regressed in 71 % of cases. Out of 13 meningiomas (5 %) which progressed, 2 were unique meningiomas. These 2 cases could represent fortuitous meningiomas without sensitivity to exogenous progestogen. The other 11 have shown growth, while other meningiomas in the same patient remained stable or regressed.
In addition, Nakamura et al published 2 reports demonstrating that meningiomas have positive growth speeds varying between 0.796 and 1.51 cm3/year. Conversely, meningiomas in our population had an average negative speed (narrowing) of -2.1 cm3/year after stopping the ACP.
We assume that these differences in meningioma growth kinetics are due to the effects of progestins. In addition, we believe that the high incidence of 29% of meningimatosis observed in our population is linked to the ACP. A similar trend has also been shown in a recent publication by Peyre et al. She suggests that the progestin induces the initiation of tumors from multiple meningeled cells.
Biological mechanism
The underlying mechanism by which ACP influences the behavior of meningiomas remains unknown.
Progesterone has been shown to have a direct positive effect on the proliferation of meningioma cells, but it can also cause increased angiogenesis and related changes in hemodynamics. with related alterations of hemodynamics. The PIK3CA/AKT1 tracks could determine the ACP mechanism, as it has recently been demonstrated that 33 % of the ACPs have changes in these signaling pathways, against only 11 % in incident meningiomas.
Limits
One of the limits of this study is the inter-judges of 2% in the measurements of the volume of meningiomas, because it is possible that subtle changes have been missed because of the average between 2 evaluators with different measures. In addition, the accuracy of the categorization of volumetric responses is also limited due to the Inter-Juges error, which leads to data loss. In addition, the accuracy of the categorization of the volumetric response is limited in the same way due to the inter-jugs error, which means that the growth or subtle narrowing in this margin of error. As this study was conceived as a series of cases, we compared our results to the previous data of the literature on the growth of meningiomas instead of an internal control group. The duration of the follow -up was 3 years on average , which means that it is not clear if the effects reported on the volumes of meningioma are durable over time. It is interesting to note that the secondary progression of a meningioma which had initially regressed was not observed in this series .
See table in the study link page 6
Implications
according to our results, the current or anterior use of a progestogen (in particular the ACP) should be systematically sought in the history of a patient with meningiomas.
In the event of prolonged exposure to the ACP for several years and in the absence of symptoms requiring urgent surgical intervention, stopping treatment should be the first option to consider . Given the frequent spontaneous stabilization and regression and the regression of meningiomas after stopping treatment, surgery or radiotherapy only seems indicated in the event of progression despite stopping the ACP. In this study, it was medically possible to stop the ACP treatment in all patients included . However, the consequences of stopping treatment are important to take into account, for example the recurrence of hyperandrogen symptoms or dysmenorrhea. Prudence must also be in order concerning the therapeutic alternatives based on progestins, such as chlormaudinone acetate or nomigestrol acetate, because some of these treatments could also promote the growth of meningiomas.
Additional research
It is necessary to obtain more data on the effect of the dose of ACP on the meningioma kinetics in order to assess whether the ACP can be continued at very low dose in the event of serious symptoms and/or psychological load. psychological.
Conclusion
We studied the behavior of intracranial meningiomas in women adult female adults who used a long -term APC were studied.
The majority of these meningiomas
- Decrease in volume (71%)
- or stabilize (19%) after stopping treatment with ACP.
Meningioma growth kinetics changes significantly, going from growth under ACP treatment to a narrowing after removal of the ACP. Consequently, the ACP seems to influence the growth kinetics of meningiomas in this population.
In the absence of symptoms requiring urgent surgery, ACP stopped could be considered the first primary treatment option for these patients.
Find our other articles here