Meningiomas
Article here:
The Menings
The mesoderm
It is one of the three embryonic sheets. It is the average sheet at the origin of the support fabric, blood, epitheliums that constitute the covering tissue, muscles, genitorerinary organs, the cardiovascular system and the coelomic cavity (pleural, peritoneal and pericardial cavities) whose coating bears the name of serous.
The Menings
They are made up of three sheets
- Pachymening or hard mother is resistant, superficial and is located at the base and on the cranial vault. It presents expansions, the brain's false, between the two brain hemispheres and the tent from the cerebellum which separates the above-mentioning space from the sub -tentoriel space (posterior pit)
- Leptomeninge includes two sheets:
- Arachnoid, from which meningiomas are born
- The Pie-Mère
They delimit three anatomical spaces:
- Extra-dural space
- The subdural space
- The subarachnoid space which contains the cephalospinal liquid (LCS), the nerves, the arteries and the veins
Meningiomas, benign tumors, but ...
A definition ...
These are slow growth tumors developed at the expense of the meninges, the envelopes of the central nervous system and more specifically from the arachnoid cells which belong to one of the three meninges sheets.
So these are tumors that develop outside the nervous (extra-cerebral) tissue.
EPIDEMIOLOGY
These are relatively frequent tumors and represent about a third of the diagnosed brain tumors. Meningiomas can, in around 5 % of patients, be multiple.
The incidence of the disease increases with age and goes from 0.3 in children, to 8.4 in the elderly.
The meningiomas are encountered, in three quarters of cases in women between 30 and 50 years old. The incidence is in women against 3.8 in humans, per year and per 100,000 inhabitants.
In addition, in about 1 % of brain MRIs made for other reasons, small non -symptomatic meningiomas are discovered.
Their topography
Most meningiomas (80 %) develop from the arachnoid surrounding the brain. A third sit on the convexity of the brain, a third party are parasagittal (brain false) and a third affect the base of the skull. The other locations are rarer (<15%) and can affect the Sellar region, Cavernous sinus, the sphenoid edge, the posterior pit.
They can, rarely, be intra-ventricular, without dural attachment (choroidal, island canvas, etc.) or orbital.
In less than 10 % of cases, they can affect envelopes of the spinal cord. They then mainly sit in the thoracic region.
The extradural and ectopic locations are rare. In this case, they can affect nasal cavities, oral cavity, parotid, ear, neck, lungs, skin or peripheral nerves. They are in good standing but can be multiple. In this case, we are talking about "meningiomatosis" which is seen during recklinghausen's disease. These are benign tumors in the majority of cases - 98 % of cases (grade 1). Certain histological types have marked aggressiveness and are classified grade 2 (atypical meningioma) or grade 3 (anaplastic meningioma) by the WHO.
Their evolution
Meningiomas develop very slowly, the brain can be able to adapt to their presence; Meningiomas often become very large before they cause symptoms.
Their development is superficial, hence the frequency of epilepsy attacks.
Although being benign tumors, some meningiomas can cause problems to the neurosurgeon because of their location in the brain.
Finally, meningiomas are however associated with significant morbidity, by the symptoms linked to their natural history or the morbidity of the treatments put in place.
Several risk factors are associated with the development of meningiomas
Exposure to ionizing radiation
- Meningiomas are the most frequent radio-induced radio tumors. The risk of developing meningioma is then 6 to 10 times higher than the general population.
Radio-induced meningiomas are generally multiple and more aggressive than in the general population, and with higher recidivism rates
Sex hormones
- The role of hormones (estrogens, progesterone and androgens) in the genesis of meningiomas is demonstrated . A rude to develop meningiomas was found when taking high -dose synthetic progestogens such as cyproterone acetate (Androcur ™), chlormadinone acetate (Lotéran ™) or numegestrol acetate (Lotényl ™). Studies have shown that cyproterone acetate multiplies the risk of meningioma in seven in seven women treated in high doses with this medication.
Family syndromes
- You should know that the majority of meningiomas appear sporadically. Nevertheless, certain family syndromes are associated with the development of meningiomas:
- There type 2 neurofibromatosis (NF2)
- It is family syndrome is an autosomal dominant disease caused by a mutation in the NF2 . Half of the patients will develop meningioma during their lifetime. The meningiomas of NF2 patients are generally multiple, early (with an average age of discovery at 30 years), and can belong to all the grades of the WHO.
- THE Gorlin syndrome
- It is an autosomal dominant disease linked to an activating mutation of one of the components of the Sonic Hedgehog pathway ( PTCH1) which associates the development of basceallular carcinomas, medulloblastomas and a meningiomal development overhaps. Five percent of affected patients have meningiomas
- Family syndromes associated with changes in SMARCB1 And SMARCE1, subunits of the complex reshaping chromatin SWI/SNF
- The germinal mutations of these genes are the cause of family forms of meningioma. Patients with germinal mutations of SMARCE1 more readily present intracranial meningomes with clear cells and spinal meningiomas, affecting the envelopes of the spinal cord.
- Other syndromes are associated with a gorgeousness to develop meningioma
- The syndromes of Cowden, Proté, Li-Fraumeni , Turcot, Gardner, Rubinstein-Taybi, and Multiple Endocrine type 1 neoplasia (NEM1)
- There type 2 neurofibromatosis (NF2)
Symptoms and diagnosis
Symptoms
The symptoms revealing meningiomas are not specific. They depend as for all the other tumors of their development topography, and are linked to the compression of adjacent neurological or vascular structures. Symptoms are a function of the location of the tumor.
The most frequent leading to diagnosis are headache, paralysis of the cranial nerves, a crisis of epilepsy, a cognitive disorder, a paralysis, dizziness, ataxicate disorders, sensitive disorders, exophthalmia.
Medical imagery
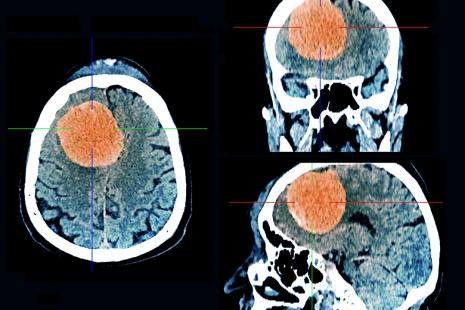
Meningiomas are generally diagnosed thanks to a scanner or a cerebral or medullary MRI with injection of contrast product.
They come in the form of a lonely rounded mass developed at the expense of the dura-mother, and are associated with a very high enhancement after injection of contrast product.
The most frequent locations are:
- Convexity in more than a third of cases (compared to the lateral side of brain hemispheres)
- In the middle (para-Sagittal compared to the medial side of cerebral hemispheres
- The base of the skull in half of the cases,
- More rarely, spinal (spinal cord), intraventricular (cavities inside the brain containing spinocellular fluid), orbital
WHO classification
| Grade i | Grade II | Grade III | |
|---|---|---|---|
| Histological subtype | Transitional fibroblastic meningothelial Psammotal angiomatous microchysics secretory rich in metaplasic |
Clear cell atypical chordoid |
Anaplastic rhabdoid papillary |
| Diagnostic criteria | <4 mitoses by 10CFG | 4 to 19 mitoses per 10CFG or cerebral invasion or 3 of the 5 elements: loss of architecture/high NC ratio/prominent nucleoles/hypercellularity/necrosis |
> 20 mitoses per 10CFG or clever appearance (carcinomatous, sarcomatous, melanocytic) |
| Main associated genetic events | Mutations NF2, Traf7, Pik3ca, KLF4, AKT1, SMO, Polr2a Loss 22Q |
Mutations NF2, Traf7, SMARCB1, SMARCE1, TERT Loss 1P, 6Q, 10Q, 14Q, 18Q GAIN 1Q, 9Q, 12Q, 15Q, 17Q, 20Q |
Mutation NF2, Tert BAP1 Loss 9P ( CDKN2AB ) Amplification 17q Loss H3K27ME3ME |
| 10 -year survival rate | 96 % | 90 % | 30 % |
| Recurrence rate at 5 years | 6 % | 17 % | 30 % |
These are benign tumors but ...
These are benign tumors
They are frankly in 98 % of cases (grade 1). Certain histological types have marked aggressiveness and are classified grade 2 (atypical meningioma) or grade 3 (anaplastic meningioma) by the WHO.
Their evolution
Meningiomas develop very slowly, the brain can be able to adapt to their presence; Meningiomas often become very large before they cause symptoms.
Their development is superficial, hence the frequency of epilepsy attacks.
Although being benign tumors, some meningiomas can cause problems to the neurosurgeon because of their location in the brain.
Finally, meningiomas are however associated with significant morbidity, by the symptoms linked to their natural history or the morbidity of the treatments put in place.
Grade WHO |
Frequency | Relapses |
|---|---|---|
| I | > 80 % | 7 – 20 % |
| II | 5 to 15 % | 30 – 40 % |
| III | < 5 % | 50 – 80 % |
Their treatment
The context
The treatment that will be proposed takes into account the size of the tumor, its location in the brain , associated signs, age and general state .
The processing methods are decided on a case -by -case basis by the medical team. The following methods can be offered to you: radio-clinical monitoring, neurosurgical excision, conventional or stereotaxic radiotherapy, and very rarely chemotherapy.
Surveillance
It is an option for small and asymptomatic meningiomas. For this, we will propose to monitor the evolution by MRI examinations.
Neurosurgery
In the general case, for symptomatic tumors and increasing in volume, the treatment is neurosurgical including at the time of recurrences which are observed in 20 % of cases recurrent at 5 years.
A complete surgical excision allows the healing of 70 to 80 % of patients.
Radiotherapy
First radiotherapy treatment is sometimes offered in the event of surgical contraindication, refusal of surgery, or in front of certain invasive meningiomas at vascular risk.
Additional radiotherapy after excision of a grade I meningioma is sometimes offered in the event of a recurrence (or the growth of a surgical residue) not accessible to surgery. The methods of radiotherapy (radiosurgery, hypo-fractional stereotaxic radiotherapy or conventional fractional radiotherapy) depend on the volume of the lesion and its proximity to risky organs.
In case of grade III meningiom, the risk of recurrence is high and radiotherapy is systematically proposed by adjuvant to surgery, regardless of the degree of excision. It is administered in the form of fractional radiotherapy.
Sometimes an adjuvant treatment ...
In cases of inconsistent tumors, such as those of the cavernous sinuses or those extended with interesting dungtriation of the venous and/or high grade systems, 3D or stereotaxic conformational radiotherapy can be offered.
Irradiation adjuvant treatment is an option for grade II and systematic meningiomas for grade III tumors.
A recurrence
One in five meningioma would repeat within ten years of the intervention. Base tumors repeat once in two in 10 years.
The causes of recurrences are still poorly understood. The age of the patient was accused, the characteristics of the tumor, still poorly known, as well as to the quality of the excision.