Summary
Aim
Methodology
Results
Conclusions
Introduction
Brain metastases appear in approximately 30% of cancer patients. In patients with a limited number of brain metastases, stereotaxic radiosurgery (SRS) is now the norm of care because it leads to less neurocognitive toxicity compared to complete brain radiotherapy. Stereotaxic radiosurgery produces high doses of radiation in a defined intracranial target using precise targeting, characterized by a clear drop in dose to target limits, reducing the damage to the surrounding tissues as much as possible. Small to medium -sized brain metastases are well treated well by stereotaxic radiochurgery because they are generally well delimited to imaging, and non -infiltrating spherical tumors.
Stereotaxic radiosurgery by scalpel gamma leads to radiation in accordance with intracranial targets. Traditionally, the precise administration of radiation by scalpel gamma has been facilitated by the leksell coordinate frame (LCF), rigidly fixed by four pin to the patient's skull. Although the LCF based on a framework gives excellent immobilization, it is invasive, is considered to be a traumatic experience for patients, and limits the use of multi-fraction treatments. Recently, our center has developed a conical beam volumetric imaging system (CBCT) to measure and treat uncertainties on gamma scalpel, guaranteeing precise positioning of intracranial targets. In turn, the availability of volumetric imaging with conical beam has enabled the development and use of a new framework of immobilization without a frame consisting of a thermoplastic mask with an infrared optical monitoring of a patient's nasal marker. The initial clinical evaluation has shown that the intra-fraction movement of the nose and the target is submillimetric when using this frameless mask system, comparable to the volumetric imaging tool with conical frame based on frame.
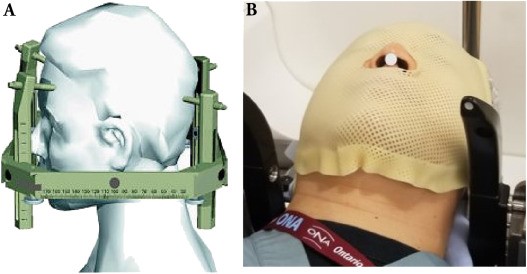
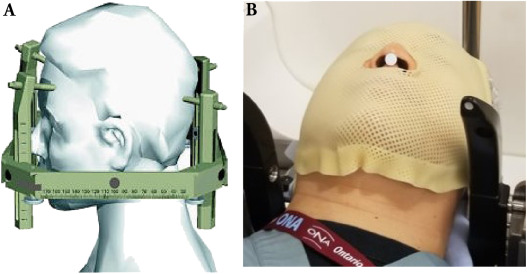
Fig. 1 mobilization of mobilization used on the gamma scalpel. (A) The leksell coordinates frame, surgically fixed at the patient's head by 4 pin. (B) The specific thermoplastic mask, manufactured during simulation and used for subsequent treatment fractions.
With the hypothesis that the immobilization devices with and without frames ensure equal accuracy and accuracy, stereotaxic radiochuruse by gamma scalpel, when clinically appropriate, patient preference can be used to guide the use of one device compared to the other. Patient opinion and level of satisfaction can be used to measure the overall quality of health care and the general satisfaction of patients is associated with a decrease in anxiety, increased compliance and improvement of results. Although the patient's perspective through a qualitative question is an essential consideration when implementing a new technology, it is not easily considered as a priority for radiotherapy research. However, qualitative analysis can provide irrefutable evidence to improve and stimulate the practice of radiotherapists. For example, studies carried out from the patient's point of view have provided useful information ranging from the assessment of immobilization comfort, monitoring preferences in a context of palliative care, and the first experiences of gamma scalpel patients in our institution. The evaluation of patient experience in the introduction of new technologies is precious, as patient experience has been shown to be linked to overall results.
At the cerebral metastase clinic of our institution, patients are sorted by a multidisciplinary team including radio-oncologists and neurosurgeons, which undergo a specific immobilization device for stereotaxic radiochuruse by scalpel gamma. Among our follow -up population, at least a third of patients seen are treated again by scalpel gamma for new brain metastases. The immobilization of patients undergoing new treatment with scalpel gamma can be obtained using either volumetric imaging with conical beam based on frame, or a frame -free mask system based on clinical factors such as the size of the lesions, the number of lesions and their location. A unique opportunity therefore exists when some patients undergo stereotaxic radiosurgery by gamma scalpel both in the frame and in the immobilization devices of the mask. The main objective of this study was to describe the experience of patients who followed a framework of immobilization by frame and mask for stereotaxic radiochuruse by scalpel gamma.
Materials and methods
It was a prospective study in a single center, with the approval of the local research ethics committee. It uses a qualitative descriptive study plan, semi-structured interviews were used to assess patients who received treatment with Gamma scalpel. An interview process was used to obtain an overview and an understanding of the patient's experience, giving the participant the possibility of freely expressing their point of view.
Study participants
During the calendar year preceding this study, our cerebral metastase clinic treated approximately 250 patients, of which around 80 have undergone new treatment (that is to say a treatment of stereotaxic radiosurgery by scalpel gamma for newly discovered lesions). Among this reprocessing cohort, about half was eligible for mask treatment. Consequently, our estimate of the cohort of patients potentially eligible for the study was 40.
Patients were recruited from the cerebral metastase clinic between May 2018 and March 2019. The eligibility criteria included: being at least 18 years old, speaking English, being able to give informed consent, and patients whose current or previous treatment plans included both the frame and the mask on the gamma scalpel. According to the study plan, it was planned to register a maximum of 20 participants, given the wear.
The study was designed so that patient recruitment stops once themed saturation has been reached.
Data collection
Patients were interviewed during their regular three -month follow -up to minimize memory biases. The participants underwent a semi-structured interview by phone or face to face, facilitated by a single co-investigator (AC). The investigator had no prior interaction with patients (that is to say that he does not work clinically on the scalpel gamma system), and was an expert in the matter with qualitative research (that is to say that he facilitated interviews with patients). The interviews lasted between 30 and 60 minutes and were recorded on audio strip. Face -to -face interviews were carried out in a private office in the hospital.
To study the experiences of patients during maintenance, an exploratory phenomenological approach was used. This methodology follows an unusual agenda, but makes it possible to deepen and clarify the questions raised; The investigator was free to follow the thread of the thought of the questioned person and to explore the tangential areas that arose. Interview questions were designed to guide study conversations.
Ten questions were used in semi-structured individual interviews, focused on the fields of patient experiences, their preferences, comfort and improvements in care:
- 1
Tell me about your experience in terms of executives.
- 2
Can you describe me the biggest concern you had about the framework?
- 3
Tell me about your experience while you follow the treatment in the context.
- 4
Tell me about your convalescence period, after your treatment in the context.
- 5
Tell me about your experience with the mask manufacturing process.
- 6
Can you describe your greatest concern about the mask?
- 7
Tell me about your experience while you receive the treatment at the mask.
- 8
Tell me about your recovery time, after your mask treatment.
- 9
Was there any additional information or resources which, in your opinion, could have been useful for the placement of executives, the manufacture of masks or the scalpel treatment by gamma in general?
- 10
By reflecting on your treatments, knowing what you know now on the frame and the mask, with which device would you have preferred to receive all your treatments?
Data analysis
The recorded interviews have been transcribed word for word, without any information allowing them to be identified. All interview transcriptions were initially examined and coded by a co-investor (IL). Each interview has been assessed based on loyalty to data collection issues, and the answers were organized by question. The data were synthesized by a qualitative-descriptive analysis, which included the reading and rereading of the text of the interview recorded on audio strip to identify and separate the main ideas containing the data on the experiences of each participant and the experiences common to all the participants in the study. A thematic analysis was carried out to identify the main results. To guarantee the rigor and credibility of the conclusions, an experienced qualitative researcher carried out an audit of the analysis. Transcriptions have been revised independently by another co-investor (AC) in order to identify the themes and minimize interpretation biases. The common themes verified by the two revisers were summarized.
Results
Twenty eligible patients were approached for registration for the study, and fifteen then gave their consent. A total of twelve patients were interviewed during their follow-up meeting; Three were removed due to the deterioration of their state of health. Five patients were first treated at the mask; Three patients were treated with the framework for a subsequent treatment for stereotaxic radiochurgery by scalpel gamma the following week, while two patients were treated with stereotaxic radiosurgy by scalpel gamma after 6 months. For the seven patients initially treated with the frame, two received the mask of stereotaxic radiochurgery by scalpel gamma during the same month. The other five patients had an average period of 28 months (from 10 to 53 months) between their initial framework and the stereotaxic radiosurgery mask by scalpel gamma.
All reinforcement treatments were carried out in a single fraction, and all the mask treatments were carried out in three fractions. The procedures for setting up the frame and manufacturing the mask were carried out as part of 15-minute appointments. The time necessary to install a patient in one or the other of the devices on the gamma scalpel couch was also comparable (that is to say 5-10 min). The average duration of fraction by fraction in the frame was 58.7 min (beach from 11.0 to 240.4 min), while the average duration of fraction treatment in the mask was 35.5 min (beach from 16.4 to 115.5 min).
Face-to-face interviews (n = 5) were carried out for patients who presented themselves in person at the clinic for their follow-up appointment, while telephone interviews (n = 7) were carried out for patients who attended virtual meetings. The interviews took place between September 2018 and May 2019, and lasted 30 to 60 minutes. During the intermediate analysis, it was determined that thematic saturation had been reached, which ended the recruitment of the study.
Four themes emerged during the interviews, which focused on patient experience and preferences for each process: unexpected pain when setting up the frame, narrowness felt with the mask during treatment, patient preference for the mask compared to the frame and improvement of care.
Unexpected pain with the placement of the framework
A major theme that came out of the interviews is unexpected pain during the executive placement procedure. The main concerns of patients concerning the frame were the pain, the invasive character and its weight once placed on the patient's head (feeling of heaviness).
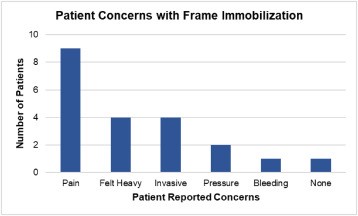
Fig. 2patients who expressed their concerns concerning the leksell coordinate frame for stereotaxic radiosurgery by scalpel gamma.
The majority of patients interviewed (7 patients) said they felt ready for the procedure. They had received brochures and educational resources on the procedure during their consultation at the cerebral metastase clinic and said it had helped them prepare for the procedure. However, 4 patients had surprises when setting up the frame. Many did not realize how much the injection of a local anesthetic and the insertion of a spindle could be painful. A patient described his experience as follows:
"You know, we say that there will be a little Lidocaine and that there will be a slight bite. It is not a slight bite, it is really painful and I still felt that the setting that was screwed was a very traumatic experience for me ”.
The patients noted that they felt a feeling of increased pressure during and after the installation of the frame. They indicated that the frame seemed heavy to them and that the feeling of pressure made the intervention very uncomfortable. Patients also said that they would have been told they would be pressure. A patient said he would have had a better experience if he had been informed of the pressure:
"I think they have given me enough information, but I would have liked to have more, that they tell me more, such as for example: you know, it will be important . And you see, just tell me in advance so that I am better prepared. Like , be more courageous and don't deflate yourself when they put it. »»
The establishment of the framework of stereotaxic radiosurgery by scalpel gamma is done in an open area of a nursing clinic, facilitated by a neurosurgeon in the presence of a medical physicist, two radiotherapists and a nurse in oncology. In our institution, a maximum of three patients are programmed for stereotaxic radiochuruse by scalpel gamma based on frame every day. While the intimacy of each patient is preserved in the clinical space thanks to pulled boats and curtains, the absence of physical barriers such as walls and a door spreads noise and conversations during the adjustment process. A patient said the physical location of the adjustment process was his greatest concern about the executive investment procedure. As other patients had their framework placed at the head of the line, their verbal reactions during the management procedure were audible throughout the space. Hearing the experiences of others before theirs was overwhelming and made the patient more nervous:
"I took an Ativan after hearing this lady shouting because I became nervous".
Several other patients have indicated that they had to take medication, such as Ativan, before setting up the framework to help them relax and calm down for the intervention.
Narrowness felt with the mask during treatment
Unlike framework -based treatments that take place on a single fraction, patients in this study cohort have undergone mask treatments on 3 fractions in addition to their mask adjustment simulation session. The main concerns of patients concerning the mask system were the ability to remain motionless and claustrophobia.
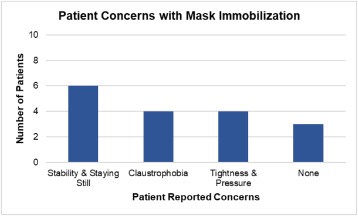
Fig. 3patients who expressed their concerns about the mask for stereotaxic radiochuruse by scalpel gamma.
Another theme that came out of the interviews is the narrowness of the mask. Four of the patients interviewed said the mask was tight and caused pain in the pressure points. A patient estimated that the pressure became unbearable after the second fraction and expressed his concerns to the radiotherapists before starting the third fraction. The patient said the radiotherapists had made adjustments to loosen the adjustment, but ten minutes after the start of treatment, the pressure was back:
"It is certain that ten minutes later, I felt extreme pressure on the right side of my head, I guess it lasted about an hour, I would say between half an hour and forty-five minutes, and I started to think that I did not know if I could bear all this time because the pressure was extreme".
Other patients felt confined to the mask because of its narrowness. Four patients said they felt claustrophobic. Some patients were worried because they had never been confined before and feared that they could not speak if they needed help. Three patients said they took medication such as ATIVAN to help them relax and make experience with the mask more bearable.
Patient preferences: mask in relation to the framework
Overall, eleven of the twelve patients interviewed preferred their experience with the mask; A patient was indifferent. Although the patients interviewed said that their treatment both with the frame and the mask was positive, ten patients had negative experience with the placement of the frame compared to a patient who had negative experience with the manufacture of the mask. In fact, half of the patients said that the mask manufacturing procedure was quite pleasant, a patient even described the procedure "as in a spa":
"I imagined it was like a facial treatment, I was able to relax and somehow enjoy it."
The patients expressed their dissatisfaction with the pain felt when installing the framework and said that the procedure was invasive. The recovery time has also been longer for the frame compared to the mask. More than half of the patients have brought back a recovery period of several days to more than a week due to bleeding at the level of the insertion sites of the pins, the healing of the wounds and the headaches due to the pressure. None of the patients interviewed reported a recovery period after treatment at the mask.
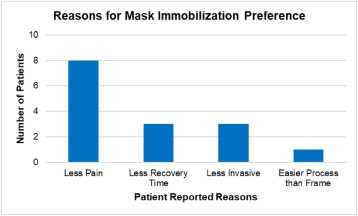
Fig. 4 Patients who indicated their preferences in terms of immobilization for stereotaxic radiochurgery by scalpel gamma.
Improvement of stereotaxic radiosurgery care by scalpel gamma
Educational resources, such as brochures, links to websites and videos, were provided to patients during consultation at the cerebral metastase clinic. The majority (11 patients) found these resources useful, but two patients said that additional resources would be desirable. According to the interviews, patients felt for the most part prepared for both framework and mask procedures, but had some surprises. A common comment was that patients were not informed of the severity of the discomfort they could possibly feel:
"Perhaps a little more information in advance than it is, you know, a little more painful. And I know, you realize that they do not want to frighten you, but I found it quite painful until it has adjusted everything and that I am good for the day. ”
Of the twelve patients interviewed, only one watched the educational video on the scalpel gamma among the three who knew the patient's education website. Three of the patients interviewed did not know what the mask would look like and a patient did not know that the frame would be surgically attached to his skull.
Discussion
Innovations in the treatment of stereotaxic radiosurgery by scalpel gamma increased its versatility in the population of patients with brain metastases. The work published to date focuses on the accuracy and accuracy of the treatment, with a minimum of emphasis on the exploration of the perspectives of the patients. The exploration of the patient's perspective in the context of the implementation of new technologies in radiotherapy is precious because it has been shown that patient experience is an indicator of the quality of care and overall results. This study explored the experiences of patients who have undergone stereotaxic radiochurgery by scalpel gamma in framework for framework by frame and mask, in order to improve care centered on the patient. From the patient's point of view, the main themes that have emerged highlighted pain concerns when setting up the frame, the narrowness of the mask during treatments, the preference of the mask in relation to the framework and a general lack of awareness of the resources available for patient education.
Patients with cancer want to be informed of their decision and treatment throughout their care path. In this study, although patients felt prepared for the procedure for setting up the framework, they expressed their surprise in the face of pain associated with the injection of a local anesthetic and the insertion of a spindle. Although the mask manufacturing procedure was favorable to patients, they were surprised by the magnitude of the discomfort felt during treatment proper because of the narrowing and adjustment of the mask:
"Maybe a little more communication as things happened. You know, "it can be hot" or "it can be tight" or "it will shrink, so the next time you come, the mask will be tight".
The participants noted in the interviews that it would be beneficial to explain the procedure at each stage without minimizing the experience. The increased use of visual aids, such as procedure videos, would be beneficial for the patient education process, in accordance with other procedures carried out in our institution.
A general theme that emerged from this study is the need to improve pedagogy towards patients and awareness of available resources. This can be partly explained by the relatively short number of days separating the initial consultation of a patient and his treatment in our cerebral metastase clinic, where patients are seen on Friday and receive treatment from the following Tuesday. If accelerated treatment is advantageous in many ways for the patient, it has the disadvantage of reducing the time necessary for patients to understand and fully assimilate the information provided regarding their processing plan. In our clinic, although individual pedagogy is carried out by experienced radiotherapists after a patient has given his consent for stereotaxic radiotherapy by scalpel gamma, and various resources are provided, patients upset by their diagnosis and their imminent treatment may not fully assimilate the information provided. This underlines the need to make the patient more aware of the educational resources, such as the institution's website link, which can be accessible remotely. Another strategy is to install patient education videos on electronic tablets that can be used independently by patients while waiting in the clinic. Telephone calls led by therapists were effective in monitoring care, a phone call to the patient one day before the intervention can represent an additional opportunity for patients to share their concerns before their stereotaxic radiotherapy by scalpel gamma.
Patients with cancer often experience anxiety, depression and distress associated with their diagnosis. Even if the placement of the frame of stereotaxic radiotherapy by scalpel gamma is associated with high stress, due to clinical factors such as the patient's history, the size and location of the tumor, stereotaxic radiotherapy by scalpel gamma based on the frame may be the preferred option for certain patients suffering from brain metastases. Effective use of patient education can reduce anxiety. Another strategy for reducing stress is to use drugs such as lorazepam preventively. To further reduce anxiety associated with the implementation of the framework, our stereotaxic radiotherapy team by scalpel gamma is actively researching another place for intervention. The placement of the frame in a closed place, far from other patients, offers greater privacy while minimizing the audible noise of the placement experience of the framework of other patients.
In this survey, patients noted a preference for the mask during stereotaxic radiotherapy by scalpel gamma, which was associated with less pain and immediate recovery compared to the frame. Since this study, we have started to offer our patients stereotaxic radiotherapy by gamma scalpel made from a single fraction mask. The first reports suggest that the mask treatment is as effective as the treatment of the frame. More extensive studies on the system of monitoring intra-fractional movements associated with the immobilization system of the mask should also strengthen confidence in its use. When clinically appropriate, the experiences and preferences of patients in this study could shed light on the immobilization used for future patients undergoing stereotaxic radiotherapy by scalpel gamma.
There are several limits which must be taken into account when interpreting the results of the study. While the patients were interviewed during their regular three-month follow-up meeting in order to minimize the memory bias, this time came from their most recent treatment of scalpel gamma. For patients who have had their framework treatment for several years before their mask treatment, this greater time gap may have contributed to their memory. Second, durations of treatment with stereotaxic radiotherapy by scalpel gamma were generally longer than the sessions in the mask due to the fractionation calendar (i.e. stereotaxic radiotherapy with a single framework in relation to stereotaxic radiotherapy with three mask fractions) and the clinical treatment approach (i.e. Compared to a single target treatment in the mask). Finally, as some patients were questioned on the phone rather than a person, this has reduced the role of non -verbal clues such as body language and visual clues.
Conclusions
From the point of view of the patients participating in this study, there was an overwhelming agreement that the immobilization by mask was the favorite choice for stereotaxic radiotherapy by scalpel gamma. The patient's experience could be improved by better pedagogy in order to better prepare the patient on what he should expect during the processes of setting up the frame and treatment of the mask.
Thanks
The authors want to underline the support of the 2016 Actrm research grant and the Robert & Andrée Rhéaume Fitzhenry program on brain metastases.
Translated by Thomas Mignaton
Source: https://www.jmirs.org/article/S1939-8654(20)30213-7/fullText
Find our other articles here