Hormonal menopause therapy and tumors of the central nervous system: Cas-Tames study in Denmark
https://pubmed.ncbi.nlm.nih.gov/38113227/
Nelsan Pouhadi, Conceptualization, Curation of data, formal analysis, investigation, methodology, project administration, validation, visualization, writing - original version, Writing and editing, 1, 2,* Amani Meaidi, Conceptualization, Curation of data, Methodology, Supervision, Validation, Writing - Revision and edition, 2 Søren Friis, Investigation, Methodology, Validation, Validation - Revision and publishing, 2 Christian Torp-Pedersen, Curation of data, Investigation, Methodology, Resources, Software, Supervision, Writing-Revision and edition, 3, 4 and Lina S. Mørch, Conceptualization, acquisition of funds, investigation, methodology, project administration, supervision, validation, visualization, writing-revision and edition 2
Summary
Context It has been shown that the use of menopausic hormone therapy containing estrogens influenced the risk of tumors of the central nervous system (SNC). However, it is not known how the progestin component affects the risk and if the continuous or cyclic treatment regimes influence the risk differently.
Methods and results
Studies CAS-TESTIMS INCRED in a national cohort of Danish women followed for 19 years, from 2000 to 2018. The cohort included 789,901 women aged 50 to 60 during follow-up, without anterior diagnosis of SNC tumor, cancer or contraindication to the hormonal treatment of menopause. Information on cumulative exposure to female hormonal drugs was based on the prescribed prescriptions. Statistical analysis has taken into account the level of education, the use of antihistamines and the use of anti-asthmatic drugs as covariable. During follow -up, 1,595 women received a meningioma diagnosis and 1,167 a glioma diagnosis. The median duration (first third quartile) of monitoring individuals in the full cohort was 10.8 years (5.0 years to 17.5 years). Compared to the absence of use, exposure to progen-progestogens or progestins alone was associated with an increased risk of meningioma, risk ratio (HR) of 1.21; (Confidence interval (CI) at 95 % [1.06, 1.37] p = 0.005) and HR of 1.28; (95 % CI [1.05, 1.54] p = 0.012), respectively. The HR corresponding to the glioma were HR 1.00; (95% CI [0.86, 1.16] p = 0.982) and HR 1.20; (95% CI [0.95, 1.51] p = 0.117). Continuous estroprogestative treatment has presented a higher meningiomal HR (1.34; (95 % CI [1.08, 1.66] p = 0.008)) that cyclic treatment (1.13; (95 % CI [0.94, 1.34] p = 0.185). The anterior use of estrogen-progenic 5 to 10 years before diagnosis Place to the strongest association with meningioma, HR 1.26; (95 % IC [1.01, 1.57] p = 0.044), while the current/recent use of progestins only gave the highest HR for meningioma 1.64; (95 % CI [0.90, 2.98] 1.83; (95 % CI [0.98, 3.41] p = 0.057).
Conclusions
The use of continuous, but not cyclical estrogens, was associated with an increased risk of meningioma. There is no evidence of an increased risk of glioma with the use of progenic estrogens. The use of a progestin alone was associated with an increased risk of meningioma and potentially glioma. Other studies are necessary to assess our results and study the influence of long -term progestogen diets on the risk of SNC tumor.
In this case-testimonial Danish, Nelsan Pouhadi and his colleagues study the influence of the progestin component of menopausic hormone therapy on tumors of the central nervous system.
The author's summary
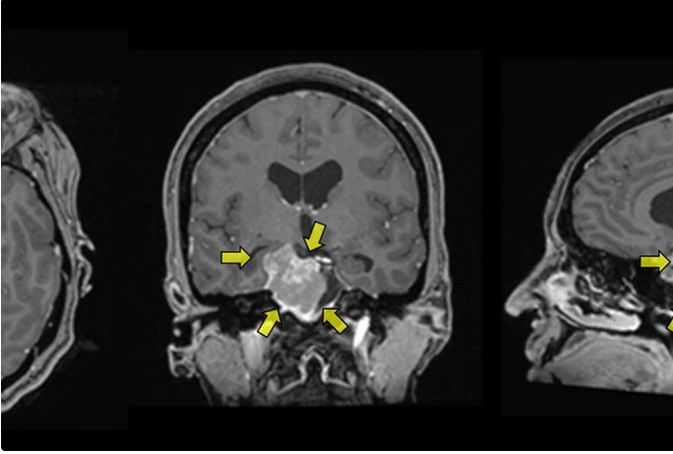
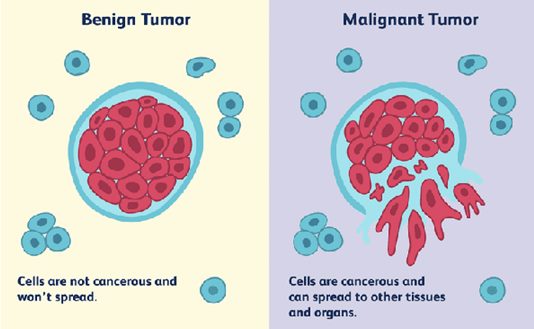
why was this study carried out? - Meningioma is the most frequent brain tumor, generally benign, while glioma is the most frequent malignant brain tumor. Meningioma is more frequent in women than in men, while it is the opposite for glioma, which suggests gender -related risk factors, such as female sex hormones (estrogen and progestin).
- previous research has shown that the use of hormonal therapy for menopause symptoms was linked to an increased risk of meningioma, but the results are not consistent with regard to the risk of glioma.
- The influence of progestin (for hemorrhagic disorders of perimenopause) and different hormonal therapies (continuous or cyclical) on the risk of brain tumor is not yet elucidated.
What did the researchers do and found?
- As part of a Danish national study based on the population, we included 789,901 women, of which 1,595 developed a meningioma and 1,167 a gliome during the study period from 2000 to 2018. The use of hormoneotherapies in women has been evaluated from the ordinances fulfilled.
- The use of continuous, but not cyclical estroprogestive therapy was associated with an increased risk of meningioma, but no glioma.
-The use of a progestin alone was associated with an increased risk of meningioma and perhaps also glioma.
What do these results mean?
- The results of this study contribute to the knowledge of the way in which brain tumors can be affected by female sex hormones, in particular progestins. Future studies should examine the role of long -term use of progestins on the risk of brain tumor.
- The results suggest that cyclic menopausic hormone therapy is a safer treatment than continuous therapy regarding the risk of meningioma.
- Due to the low use of transdermal hormone therapy among women included, we have not been able to study this form of administration. This is an observation study; It is therefore not possible to exclude uncompical influences.
Introduction
Méningiomes are the most common benign tumors of the central nervous system (SNC) and meet more frequently in women, with a women/men ratio of up to 3.5, the highest proportion being observed in average age. Conversely, gliomas are the most frequent malignant tumors of the SNC, with an incidence of 50 % higher in men. Although the etiology of these tumors is largely unknown and only a few rare risk factors have been established, the difference in incidence between the sexes indicates potential risk factors related to sex, including the exogenous use of female sex hormones.
Meningiomas and gliomas are sensitive to hormones and the two tumors express estrogen and progestogen receptors. In observation studies, oral hormone therapy based on estrogen alone, which is only recommended for hysterectomized women with vasomotor symptoms, has been associated with an increased risk of meningioma. However, the results concerning the use of the Estroprogestative association, the main hormone therapy in menopausal women whose uterus is intact, are contradictory, certain studies reporting an increased risk and others of an absence of association. Menopause hormone therapy and oral contraceptives have been associated with a reduced risk of glioma in meta-analysis, and estrogen receptors have therefore been suggested as potential target in the endocrine treatment of glioma. However, data is contradictory, other studies reporting an increased risk of glioma in estrogen users alone by systemic means.
The specific influence of progestins on the development of SNC tumors is not resolved. While we think that the risk of meningioma associated with hormone therapy is mainly due to the estrogen component, new data suggest that progestogen is an independent potential risk factor. A recent observation study reported a strong dose-answer relationship between the use by women of a progestogen with anti-diandrogenic effect and the risk of meningioma. Another recent study has revealed an increase in the risk of meningioma in the event of prolonged exposure to other progestins, thus stressing that the influence of progestins on the development of meningiomas does not seem to be limited to progestins with antiandrogen effects. The role of the progestin in the development of meningioma also indicates a potential difference in the influence of cyclic treatment compared to continuous treatment with a progestogen in the context of combined hormonal therapy. However, most previous studies have not been able to assess cyclic treatments compared to continuous treatments or have noted a similar influence on these treatments on the development of meningiomas. In addition, studies had limited statistical precision to assess the potential differential influence according to cumulative schemes. Finally, the effect of progestins on the risk of glioma is currently unknown.
In this national study based on the population, we have examined the influence of the use of menopausic hormone therapy on the incidence of meningiomas and gliomas by focusing on the use of estrogen-progestin in non-hysterectomized women, with regard to the type of diet (for example, cyclic or continuous regimes), the duration of the treatment and the status of the user. In addition, we have evaluated the associated incidence of meningioma or glioma with the use of estrogen therapy alone in a population of hysterectomized women.
Working methods
population studied by coupling of Danish national registers, we have identified an open national cohort of Danish residents aged 50 to 60 years in 2000 or having reached the age of 50 between 2000 and 2018. Women were followed either from January 1, 2000, or from their 50th anniversary during the study period from January 1, 2000 to 310 December 2018. Assign a single identification number recorded in the civil status registration system, which allows data to be linked without ambiguity to the individual level. The national cohort was based on the following registers: (1) the Danish cancer register; (2) The national patient register; (3) The national register of prescriptions; and (4) the Danish register of education. An earlier diagnosis of meningioma, glioma or cancer (except melanoma -free skin cancer) has led to exclusion. We have also excluded women with contraindications to menopausic hormone therapy, including an earlier diagnosis of stroke, acute myocardial infarction, venous thrombosis, liver disease or thrombophilia. The main exposure we are interested in was Estroprogestive combined therapy, used by women whose uterus is intact, the progestin component being administered to protect the endometrium from the malignant proliferation induced by estrogens. Hysterectomized women have therefore been excluded from the main population of the study, as women without uterus should not receive a combined estroprogestative treatment for vasomotor symptoms, but rather an estrogen -based treatment only. A distinct cohort of hysterectomized women (also presenting the same characteristics as the main non -hysterectomized cohort) was identified to study exposure to estrogen treatment alone in its clinical target population. Exclusion information (that is to say diagnostics and surgical procedures) was available from 1977. Finally, we excluded women who immigrated to Denmark after January 1, 1995 (start of the register of prescriptions). Women were censored during follow -up if an exclusion criterion appeared or at the time of emigration or death.
Two separate case-testimous populations for meningiomas and gliomas were established from the national cohort. Meningiomas or incident gliomas occurring during follow -up were considered as cases. Each case was paired by year of birth by pairing of density of incidence at 10 individuals witness to the cohort who had no diagnosis of SNC tumor or censorship criterion on the date of diagnosis/pairing of the case (index date). Thus, the paired populations included risk sets (1,595 for meningiomas and 1,167 for gliomas), each being composed of a case and 10 witnesses of the same age on the index date, therefore subject to the same circumstances of potential exposure to menopausic hormone therapy.
Hormonal treatment of menopause
Data on the use of hormone therapy in the studied population has been obtained from the national register of prescriptions which provides information on all the prescriptions reimbursed by Danish pharmacies since 1995. The use of hormone therapy from 1995 and throughout the follow -up was obtained from prescription files with the therapeutic codes (ATC) relevant (Table A in text S1) and information on the associated active ingredients (type of estrogen or progestogen), the unit of medication, the size of the packaging, the administration and the date of dispensation.
Estrogen administered by systemic route is the main treatment of menopause vasomotor symptoms and, for women whose uterus is intact, treatment also includes progestin for the protection of the endometrium. Estrogen-progestogen combined treatment has therefore been the main exposure studied. Continuous use has been defined as the issuance of one or more orders for combined estroprogestive preparation (ATC G03F and unique preparation with ATC G03HB01) or simultaneous use of a systemic product based on single estrogen (ATC G03C) and a Productive Products alone (ATC G03D or the intrauterine device ATC G02BA03). In addition, continuous (ATC G03FA, DOSE DOSE DOSE of progestogen) and cyclic (ATC G03FB, progestogen at the end of a treatment cycle) treatment schemes have been identified.
To take into account the use of hormonal preparations other than the estrogen-progestogen combination, we have also recovered information on (1) the estrogen therapy alone; (2) Progestotherapy alone (used for hemorrhagic disorders of perimenopause); and (3) Vaginal estrogen (used to treat the geni-food syndrome of menopause-ATC G03CA03).
The duration of treatment of hormone therapy was calculated using the "Medicinmacro" program of the R "GitHub/Tagteam/Heaven" package. Information relating to prescription, including the date of delivery and the quantity of hormone therapy (packaging size, unit size and number of packaging), as well as the data on the dosage recommendations from the summary of the characteristics of the product served as the basis for the calculation. The treatment periods were calculated by assuming the use of the default dose recommended at the start of treatment. If a woman has obtained additional prescriptions, the program calculated (on the basis of the five most recent prescriptions) if the treatment could be continuous by assuming a minimum, maximum or default daily dose.
Women using both an estroprogestative combination and another hormonal therapy product during follow -up were classified as estroprogestative users. Women using both cyclical and continuous estroprogestatives have been classified in the category of mixed users. Estrogen users alone and progestoges alone, without the treatment periods, have been classified separately. Women who bought vaginal estrogens but no systemic hormone therapy were considered as vaginal estrogen users only. The association between the use of vaginal estradiol and the risk of SNC tumors has been reported in a separate study.
Meningioma and glioma
Meningioma was defined as the first date of validated meningioma diagnosis obtained from the Danish Danish Cancer Register (International Classification of Diseases, 10th Revision
(
CIM-10): C70.0, C70.9, D32.0, D32.1, D32.9, D42.0, D42.1, D42.9; Oncology, 3rd edition (CIM-O-3): 95300, 95301, 95303, 95310, 95311, 95313,
95320, 95321, 95323, 95330, 95331, 95333, 95340, 95370, 95373, 95381
, 95383 95393) [18].
The glioma was defined as the first date of diagnosis validated validated glioma (including multiform glioblastoma, astrocytoma gliomme multiform, astrocytoma of grade II and III, and oligodendrogliomme of grade II and III; CIM-10:
C71.0-C71.9, d33.0-d33.2, D43.0-D43.2; and CIM-3 morphology: 94403,
94003, 94013, 94113, 94503, 94513, 94603, 93801, 93803, 93813, 93823,
93831, 93900-94001, 94121-94401 94413-94501).
Although the glioma did not serve as a negative control result defined a priori in our study, we expected different associations with exposure (i.e. menopausic hormone therapy) compared to those for meningioma, as reported with previous studies. Since the results for the two SNC tumors had to have comparable biases sources, any difference in associations could probably be attributed to the exhibition.
Potential confusion factors
Age and level of education (primary school only, secondary school only, vocational education, university education, university education and doctorate) have been considered as demographic and socio-economic confusion. Due to the reverse association between allergies and SNC tumors, antihistamines (ATC R06A) and anti-asthmatic drugs (ATC R03) have been considered potential confusion factors. As a descriptive characteristics of the studied population, we have also included information on diabetes (anti -diabetic drugs), the use of statins, aspirins and NSAIDs, all defined from the orders filled.
Statistical analysis
Conditional logistics regression was used to calculate adjusted risk reports (RR) and 95 % confidence intervals (CI) for associations between hormone therapy and meningioma or glioma in the two paved populations.
In the main analysis, the exposure has been grouped according to the type of hormone therapy: (1) No use (reference); (2) Progenic estrogen (continuous or cyclical subdivided); (3) estrogen alone; (4) progestin alone; and (5) vaginal estrogen alone. In secondary analyzes, we have examined the associations between the cumulative duration of treatment (≤1 year;> 1-4 years;> 4 years) by continuous estrogen-progestom, cyclic and progestin-progestogen alone and the risk of meningioma and glioma.
The status of user of hormone therapy was evaluated in a separate analysis and defined according to the last day of treatment before the date of the index: (1) current/recent 0 to 2 years (last day of treatment within 2 years before the date of the index); (2) Anterior> 2-5 years (last day of treatment in 2 to 5 years before the date of the index); (3) earlier> 5-10 years (last day of treatment within 5 to 10 years before the date of the index); and (4) earlier> 10 years (last day of treatment before 10 years before the date of the index).
Systemic estrogens are used by women who have no uterus. Consequently, a distinct analysis has evaluated the association between the use of estrogens alone by systemic route and the risk of meningioma or glioma in the clinical target population, that is to say women hysterectomized.
A one year offset window before the date of the index (that is to say the omission of any prescription of hormone therapy in the year following diagnosis/pairing) was systematically applied in all analyzes in order to reduce the possibility of a reverse causal bias. All the analyzes were also carried out with a two -year gap without gap as sensitivity analyzes.
We carried out post-hoc sensitivity analyzes among women aged 50 to 55 between 2000 and 2018. The oldest women in this subpopulation were 50 years old in 1995 (start of the prescription register), which allows an almost complete assessment of exposure to menopausal hormone therapy at the age of menopause.
All analyzes have taken into account the level of education, anti-asthmatic drugs and antihistamines as covariable and were carried out using statistical software R, R Core Team (2020). Bilateral P values were calculated using the Wald test. The values P below 0.05 were considered significant.
This study has been reported in accordance with the Strobe guideline (Strengthening the Reporting of Observational Studies in Epidemiology).
Declaration of ethics
Danish law stipulates that studies based on national registers in Denmark do not require ethical approval or patient consent. This study was approved by the Danish Data Protection Agency (Approval ID: P-2019-280) and the Danish Health Data Council (Approval ID: FSEID-00005931).
Results
The national cohort included 789,901 eligible women followed for 8.5 million people with a median follow-up period (first third quartile) of 10.8 years (5.0 years to 17.5 years). During follow -up, meningioma was diagnosed in 1,595 women (0.20 %) and a glioma in 1,167 women (0.15 %). The constitution of the cohort and the overwhelmed case-testimous populations is presented in the image 1. The median age at the time of the diagnosis of meningioma and glioma was 60 years (56 to 66 years). The characteristics of cases and witnesses in the two paired populations are specified in Table 1.
Image 1
Organizational chart of the establishment of the cohort and the overwhelmed case-to-withered populations.
Table 1
Characteristics of the two paired populations.
| Meningioma ( n = 1.595) | Controls ( n = 15.950) | Glioma ( n = 1.167) | Checks ( n = 11.670) | ||
| Age at the time of diagnostic/pairing - median (years) | 60 (56–66) | 60 (56–66) | |||
| Median duration of follow -up (years) | 8.9 (4.5–13.6) | 8.1 (3.7–12.3) | |||
| Year of diagnosis / average of the pairing | 2013 (2008–2016) | 2011 (2007–2015) | |||
| Use of hormone therapy | |||||
| Estrogen-progesting | 423 (26.5) | 3,785 (23.7) | 277 (23.7) | 2,827 (24.2) | |
| Continuously | 108 (25.5) | 872 (23.0) | 56 (20.2) | 624 (22.1) | |
| Cyclic | 170 (40.2) | 1,636 (43.2) | 131 (47.3) | 1,264 (44.7) | |
| Mixed | 129 (30.5) | 1,098 (29.0) | 76 (27.4) | 771 (27.3) | |
| Unknown | 16 (3.8) | 179 (4.7) | 14 (5.1) | 168 (5.9) | |
| Estrogens only | 33 (2.1) | 284 (1.8) | 21 (1.8) | 223 (1.9) | |
| Progestogy only | 143 (9.0) | 1,203 (7.5) | 99 (8.5) | 849 (7.3) | |
| Vaginal estrogen only | 215 (13.5) | 2,120 (13.3) | 155 (13.3) | 1,483 (12.7) | |
| Estrogen alone and progestin alone | <4 (<0.3) | 38 (0.2) | 4 (0.3) | 27 (0.2) | |
| Age at the start of the disease - median (years) | |||||
| Hormonal treatment of menopause | 50 (47–53) | 50 (46–52) | 50 (47–53) | 50 (46–53) | |
| Vaginal estrogen | 56 (53–60) | 56 (53–60) | 56 (52–59) | 56 (53–60) | |
| User status (hormonal treatment of menopause) | |||||
| Current user/recent 0-2 years | 143 (23.8) | 1,236 (23.3) | 103 (25.7) | 1,056 (26.9) | |
| Previous user> 2-5 years | 85 (14.1) | 752 (14.2) | 56 (14.0) | 602 (15.3) | |
| Previous user> 5-10 years | 149 (24.8) | 1,261 (23.7) | 95 (23.7) | 1,023 (26.1) | |
| Previous user> 10 years | 230 (38.2) | 2,150 (40.5) | 152 (37.9) | 1,312 (33.4) | |
| Level of education | |||||
| Primary school | 473 (29.7) | 5,225 (32.8) | 407 (34.9) | 3,875 (33.2) | |
| College and high school | 45 (2.8) | 424 (2.7) | 32 (2.7) | 299 (2.6) | |
| Vocational education | 668 (41.9) | 6,459 (40.5) | 476 (40.8) | 4,621 (39.6) | |
| University education | 325 (20.4) | 3,140 (19.7) | 206 (17.7) | 2,335 (20.0) | |
| University and doctorate | 84 (5.3) | 702 (4.4) | 46 (3.9) | 540 (4.6) | |
| Health -related variables | |||||
| Diabetes | 118 (7.4) | 991 (6.2) | 73 (6.3) | 644 (5.5) | |
| Asthma | 530 (33.2) | 5,011 (31.4) | 366 (31.4) | 3,474 (29.8) | |
| Statins | 397 (24.9) | 3,259 (20.4) | 238 (20.4) | 2,199 (18.8) | |
| Aspirin | 247 (15.5) | 1,893 (11.9) | 154 (13.2) | 1,267 (10.9) | |
| Antihistamine | 589 (36.9) | 5,539 (34.7) | 381 (32.6) | 3,779 (32.4) | |
| NSAID | 1,268 (79.5) | 12,217 (76.6) | 914 (78.3) | 8,794 (75.4) | |
Values expressed in number of women (%) or in the middle (first third quartile).
User status defined according to the last day of treatment before the date of the index: (1) current/recent 0-2 years-within 2 years preceding the date of the index; (2) Anterior> 2-5 years-within 2 to 5 years preceding the date of the index; (3) Anterior> 5-10 years-within 5 to 10 years preceding the date of the index; and (4) earlier> 10 years - before the 10 years preceding the date of the index.
Combined estrogen-progenic users represented 26.5 % of meningioma cases (23.7 % of witnesses) and 23.7 % of gliomas (24.2 % of witnesses), with a median age at the start of treatment of 50 years (47 to 53 years). The majority of users of menopausic hormone therapy had their last day of treatment less than 5 years before the date of the index.
Among the cases of meningioma, 25.5 % of the users of progen-progestogens were exposed to a continuous progestogen, while 40.2 % were exposed to a cyclic progestogen. For gliomas, the corresponding prevalences were 20.2 % and 47.3 %. About a third of all users of procurean estrogen had either tried continuous and cyclic treatment (27.3; 30.5%), or could not be categorized reliably (3.8; 5.9%).
Of all of the years of use of menopausic hormone therapy in the cohort, 90.3 % were administered orally, 7.9 % by transdermal route and 1.8 % by other paths of administration (Table A in text S1). Estradiol was the most used estrogen type (> 96% of the use of estrogens). The most frequently used progestins in desktoprogestative combined products were norethisterone (74 %) and medroxyprogesterone (13 %).
Progestin users alone represented 9 % of meningiomas and 8.5 % of gliomas cases. Among the progestogen preparations used, 68 % contained medroxyprogesterone, 14 % norethisterone and 12 % of levonorgestrel (intrauterine device). The detailed details of the use of hormone therapy in the cohort are specified in Table A in text S1.
The use of hormonal treatment according to the type and associations with meningioma and glioma are presented in image 2. With regard to the absence of use, the use of progenic estrogens has been associated with an increase in meningioma HR of 1.21; (95 % CI [1.06, 1.37] p = 0.005), but no HR glioma 1.00; (95 % CI [0.86, 1.16] p = 0.982). Continuous estroprogestative treatment has been associated with a moderate increase in meningiomal HR of 1.34; (95 % CI [1.08, 1.66] p = 0.008). Cyclic treatment has shown associations close to the unit for the meningiom of 1.13; (95 % CI [0.94, 1.34] p = 0.185) and the HR 1.05 glioma; (95 % CI [0.86, 1.29] p = 0.616). The use of a progestogen alone was associated with a slight increase in HR for meningioma 1,28; (95 % CI [1.05, 1.54] p = 0.012) and glioma 1.20; (95 % CI [0.95, 1.51] p = 0.117).
2 hrs image
of the use of hormone therapy and associations with SNC tumors.
Folder note: In a distinct cohort of hysterectomized women, exposure to estrogen alone gave an HR of 1.22; (95 % CI [0.90, 1.66] p = 0.20) for meningioma (122 cases and 1,179 witnesses) and 0.81; (95 % CI [0.55, 1.18] p = 0.27) for glioma (65 cases and 632 witnesses) (Table B in text S1). Estimates of exposure to non -riding treatments based on estrogen alone and progestins, to mixed or unknown treatments based on estrogen and progestins, and to vaginal treatments based on estrogen alone are presented in Table C of part S1 of the text. Adjusted according to the level of education and the use of anti-asthmatic drugs and antihistamines. IC, confidence interval; SNC, central nervous system; HR, risk report.
In the distinct cohort of hysterectomized women, the use of estrogens alone by systemic route gave an HR of 1.22 (95 % CI [0.90, 1.66] p = 0.203) for meningioma (122 cases and 1,179 witnesses) and an HR of 0.81 (95 % CI [0.55, 1.18] 0.267) for glioma (65 cases and 632 witnesses) (Table B in text S1).
Image 3 shows HR for meningiomas and gliomas as a function of the cumulative use of estrogen and progestogen and the use of progestins alone. The cumulative use of continuous-progogens-progesting has been associated with an increase in HR for meningioma, but not according to a coherent period-answer scheme. The cumulative use of cyclical estrogen-progestogens has not been associated with the risk of meningioma. The duration intervals of estroprogestative treatments were not associated with the risk of glioma. Although statistical accuracy is limited, the use of a progestogen alone has been associated with high estimates of the risk of meningioma which increased with the cumulative duration of treatment. For glioma, no coherent period-response plan has been observed with the cumulative use of progestins alone.
Image 3
hrs of the cumulative use of estrogen-progestin and progestins alone and association with SNC tumors.
Futorial note: adjusted according to the level of education and the use of anti-asthmatic drugs and antihistamines. SNC, central nervous system; HR, risk report.
Image 4 shows associations between meningiomas and gliomas and the use of estrogen-progestin depending on the status of the user (current/recent anterior versus), the previous use 5 to 10 years before the index date showing the strongest association with the HR 1.26 meningiomas; (95 % CI [1.01, 1.57] p = 0.044). The current/recent use of a progestogen alone presented the highest HRs for the HR 1,64 meningioma; (95 % CI [0.90, 2.98] p = 0.104) and HR glioma, 1.83; (95 % CI [0.98, 3.41] p = 0.057). The status of estrogen user alone has not been systematically associated with meningioma, but the current/recent use gave the highest estimate: HR, 1.91; (95 % CI [1.00, 3.65] p = 0.050).
Image 4
hrs of the use of hormone therapy and SNC tumors according to the status of the user.
Luts note: User status is defined according to the last day of treatment before the date of the index: (1) Current/recent 0-2 years-Environ 2 years before the date of the index; (2) Anterior> 2-5 years-Environ 2 to 5 years before the date of the index; (3) Anterior> 5-10 years-Environ 5 to 10 years before the date of the index; and (4) anterior> 10 years-environment 10 years before the date of the index. Adjusted according to the level of education and the use of anti-asthmatic drugs and antihistamines. SNC, central nervous system; HR, risk report.
Associations remained largely unchanged in sensitivity analyzes with a two-year discrepancy and without gap (images A to F in text S1) as well as in post hoc sensitivity analysis in a subpopulation with an almost complete exhibition history around the age of menopause (Table D in text S1).
Discussion
in this national study based on the population and nested in a cohort of peri- or post-menopausal women, the use of progening estrogens was associated with an increased risk of meningioma, when there was no evidence of an increased risk of glioma. The association for meningioma was limited to the continuous use of progening progening. The anterior use of estrogen-progestogens, up to 10 years before the diagnosis, was associated with an increased risk. High risk estimates have also been observed for the use of progestins alone and the risk of meningioma and perhaps also glioma. The use of estrogens alone by systemic route has not been associated with the risk of glioma, but a slight increase in the risk of meningioma has been observed for processing by estrogen alone by systemic route.
Estrogen and progestogen receptors are present in meningiomas and gliomas, so that exposure exogenous with female sex hormones could have an impact on tumor growth. The increase in the risk of meningioma observed in women using hormonal treatment of menopause in previous studies has been mainly attributed to the estrogen component, because stronger associations have been found with the use of estrogens alone than with the use of an estrogen-progestogen combination. However, we have found coherent associations for meningiomas with the continuous use of progenic estrogen and, in addition, with the use of progestins alone. Meningiomas express more progestin receptors than estrogenic receptors (88 % against 40 % in an immunohistochemical analysis; therefore, the use of progestins can possibly influence the development of meningiomas. Continuous combined hormone therapy includes a daily dose of progestogen, while cyclic therapies Progressive than at the end of a treatment cycle. A slight increase in the ODDS ratio (gold) adjusted (1.5; 1.0 to 2.2) for meningiom in the event of continuous use of estrogen -rogestatives, but not in the event of cyclic use (1.1; 0.7 to 1.6). In addition, in accordance with the results of two recent observational studies (2020 and 2021) on exposure to exogenous progestins and the risk of meningiom, we have found an increase in meningioma level in women using progestin -based preparations only.
Continuous estroprogestative treatment, as defined in this study, does not include the intrauterine device releasing levonorgestrel. Although it can be used as a continuous progestogen component in combined hormone therapy for menopausal women, we did not have sufficient statistical accuracy to examine the use of systemic estrogens combined with the intrauterine system for liberation from Lévonorgestrel and associations with meningioma. This aspect should therefore be assessed in future studies.
The results of our study contribute to the understanding of the etiology of brain tumors by highlighting the progestin component of hormonal therapy products as a potential risk factor of meningioma and perhaps also glioma. In addition, although absolute risks can be relatively low due to the scarcity of SNC tumors, our results suggest that cyclic-progesting estrogen is safer therapy regarding the risk of meningioma. The growing number of evidence regarding the risk of meningioma linked to the use of progestins by women calls for scientific attention.
A recent meta-analysis (2018) reported a reduction in the risk of glioma with the use of menopausic hormone therapy, but called for the realization of other studies with greater samples to deepen the results. In accordance with an anterior observational study, we found a generally neutral association between the use of menopausic hormone therapy and the risk of glioma.
In particular, the current/recent use of menopausic hormone therapy has been associated with a high risk of meningioma, while previous use has not revealed an increased risk. However, most previous studies were based on relatively short monitoring periods. In our study, we have noted an increased risk of meningioma both in current/recent user of estrogen-progestin for previous users (up to 10 years before the diagnosis of meningioma). An explanation possible of the differences in results concerning the previous use is that a prolonged follow -up period and larger samples, as in our study, are probably necessary to examine the influence of the moment of exposure, which is crucial in slowly evolution results as well as meningioma.
Numerous studies based on registers and relating to associations between the use of hormonal treatment of menopause and the development of SNC tumors have included women aged 75 to 89 in their study populations. Consequently, these studies have not evaluated the relevant exposure around the perimeneopausic age for a significant proportion of the women included, which led to an underestimation of exposure in the studied population and a erroneous classification of users as non-users, thus attenuating potential associations between the use of menopausic hormone therapy and the risk of SNC tumor.
Among the strengths of the study are the importance of the national sample with long -term continuous monitoring, very valid meningioma and glioma diagnoses and detailed information on the use of hormone therapy. The Danish register of prescriptions provides complete data on the prescriptions executed from 1995; Consequently, only women aged 50 to 60 between 2000 and 2018 were included. Age restriction has made it possible to detect the use of hormone therapy around the age of menopause for most of the women included, thus reducing the bias towards zero value in many previous observation studies.
This study has limits. First of all, only a small proportion of women in Denmark used transdermal hormonal therapy and few of them were long -term users of a progestogen alone. Consequently, we were unable to assess the influence of administrative modes or long -term use of progestins alone on the occurrence of SNC tumors. Associations between the use of progestins and the risk of SNC tumor are likely to postpone according to the type of progestogen. In our study, 74% of the total use of combined treatment contained norethisterone (13% contained medroxyprogesterone) and 68% of the total use of progestogen alone contained medroxyprogesterone (26% contained either norethisterone, or levonorgestrel).
Second, since the prescription register started in 1995, we could not detect exposure to hormone therapy before 1995, which could lead to an underestimation of the associations observed. However, a post hoc sensitivity analysis on women whose exhibition history was almost complete confirmed our main results.
Likewise, information on the past use of hormonal contraceptives before 1995 was not available. It is therefore not possible to exclude any potential confusion, since the former users of hormonal contraceptives were more likely to have recourse to menopause hormone therapy.
Finally, due to the observational nature of the study, we cannot exclude residual confusion due to unbeknown or unknown risk factors for SNC tumors. However, many factors related to lifestyle have been the subject of in -depth studies and have not had an impact on the risk of meningioma or glioma; We therefore do not think that the residual confusion factors had a major influence on our results. In addition, we expect the two results of our study (that is to say meningioma and glioma) largely share the same sources of residual biases and measured and not measured factors. Our observation that associations with meningioma and glioma were substantially different makes it possible that the difference is the result of the exposure (that is to say hormone therapy), thus reinforcing the probability of a causal link between the use of menopausic hormones and the results.
Due to its design, an overwhelmed case study with an appropriate matching of incidence densities provides the same rate reports as if the complete cohort was analyzed in a prospective manner. However, the absolute risk estimation was not possible in the context of an overwhelmed case study.
In conclusion, the use of progening estrogens has been associated with an increased risk of meningioma, regardless of the status of the user (current/recent or old), while there was no evidence of an increased risk of glioma.
Continuous, but non -cyclical estroprogestative treatments were systematically associated with an increased risk of meningioma . The use of progestins alone has been associated with the risk of meningioma and potentially also with the risk of glioma. The use of estrogens alone by systemic or vaginal route has not been associated with the risk of glioma, but estrogens alone by systemic means can be associated with the risk of meningioma.
Other studies are necessary to assess our results and explore the long -term use of progestins alone and the risk of SNC tumors, since this study suggests a role of progestins in the etiology of SNC tumors.